Case Study — Florida Blue
Concierge Service Model
A tailored set of tools used for a specialized team to identify at-need patients and offer targeted resources and information for their condition.
Discovery
As more health insurance providers enter the market, consumers increasingly expect best-in-class, personalized service. Florida Blue invested in the Care Consulting Team (CCT): a specialized group of about 40 "super-users" whose focus is being the first point of contact for members recently diagnosed with a chronic condition — Diabetes, Hypertension, Asthma, COPD, or CHF.
The problem: the IVR system was routing the wrong calls to these specialists. CCT advocates were receiving billing and claims calls instead of the complex health-related calls they were trained for. To fix this, I worked with the business and IVR team to create special routing rules. We identified a target population of about 4,000 members in the Orlando area as a pilot group — when a CCT advocate opens CustomerConnect for one of these members, they see a specialized Concierge view.
Research
Over 8 weeks, I met with a focus group of CCT experts to conceptualize a new tool to help them quickly understand where a member was in their health journey.
A critical insight emerged early: the success metric for this tool would be Quality scores, not Average Handle Time. If the right members were on the phone, AHT would actually increase — because the conversations needed to be substantive. This drove every design decision.
I created discussion guides to drive focus group conversations and validate which data points CCT advocates actually needed. We found that presenting information in a linear path helped advocates ask probing questions to determine if a member was suited for special programs.
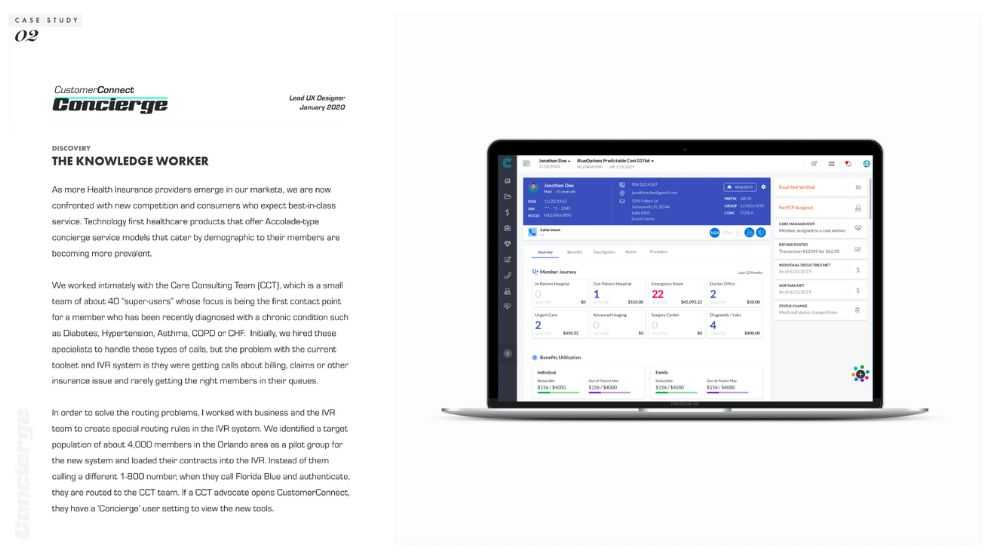
The three essential views:
- Episode History — quickly shows which types of care the member is using
- Benefits Utilization — shows how close the member is to meeting their Deductible or OOP Max
- Pre-Service Authorizations — assists in preventing high-cost visits (e.g., MRI at a hospital vs. a Diagnostic Imaging facility)
Testing & Prototyping
When we conceptualized how the business could intervene and redirect members toward appropriate care, we developed a model for proactive outreach. The Concierge Roster was born — a tool for leadership or the CCT team to filter the population by specific data points and find members fitting specific criteria.
The Roster can quickly filter for members who are high utilizers of benefits, have no PCP assigned, or have chronic conditions. These lists can be loaded into the IVR for Specialty advocates, used for SMS/mail campaigns, or to refer members to Care Programs.
Testing both tools side-by-side with the focus group was powerful. Listening to a phone call where a member was out of the area and recently diagnosed with Cancer made the stakes completely real. The level of support and empathy this team provides is exactly what drives me to give them the best tools possible.